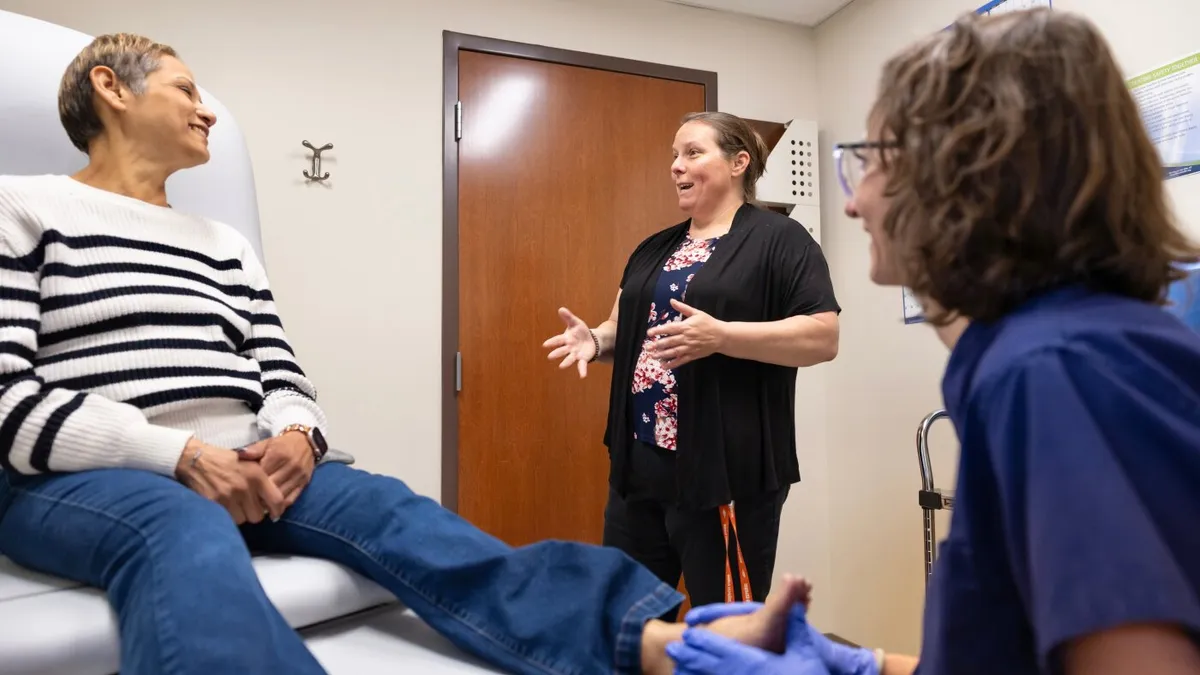
Maria Olivo grew up in Rifle, Colorado, a town where about 36% of people speak Spanish at home. From age five or six, she interpreted for her mother at banks and doctor's offices. This was a heavy responsibility for a child. Olivo often worried she might get something wrong.
"I'm pretty sure that a lot of it I messed up," Olivo said. "I wasn't sure half of the time, right? I was just a kid."
She continued interpreting for 12 years, always hoping she used the correct words. Eventually, Olivo refused to interpret for her mom at the gynecologist's office. She realized that medical conversations need someone with proper terminology, not just a family member.
We're a new kind of news feed.
Regular news is designed to drain you. We're a non-profit built to restore you. Every story we publish is scored for impact, progress, and hope.
Start Your News DetoxOlivo now works as a quality analyst at Grand River Health, Rifle's 57-bed hospital. She has seen other families face similar communication issues. In 2023, focus groups with Hispanic and Latino community members told hospital staff that language barriers caused confusion and made them feel unwelcome.
The Dangers of Poor Interpretation
Poor interpretation can lead to serious medical errors and a higher risk of lawsuits, according to Dr. Glenn Flores. He chairs pediatrics at the University of Miami's Miller School of Medicine and has studied this issue for decades. Small language differences can have critical consequences.
Dr. Flores noted cases where children died because siblings acted as interpreters. Patients are also less likely to be honest about sensitive topics like drug abuse or domestic violence when family members are present. Sometimes, hospitals even rely on untrained staff or people from local restaurants to interpret.
Grand River Health's Solution
A couple of years ago, Grand River Health decided to change this. They hired a language access coordinator and a full-time medical interpreter. They also started offering formal training to their bilingual staff to become qualified interpreters. Dozens of employees have completed the 40- to 60-hour course.
Dr. Kevin Coleman, Grand River's chief medical officer, admitted he used to rely on family members for interpretation. He now finds this embarrassing.

These dual-role employees, who might be receptionists, radiologists, or medical assistants, now interpret for Spanish-speaking patients a few times a day. They receive a small pay increase based on their training and certification. Even with these costs, Dr. Coleman says the program saves the hospital money.
Grand River used to spend much more on virtual interpretation services. Now, they use virtual services less often and pay about a third of the previous cost. The hospital has also seen about 50% more Spanish-speaking patients since the program began two years ago.
Dr. Coleman hopes Grand River's success will encourage other hospitals to improve their language services. He believes the program, despite its initial costs, has paid off well.
The program still uses virtual interpreters for languages other than Spanish, and during nights and weekends. Sometimes, these virtual interpreters speak a different dialect than the patient. Some dual-role employees initially felt overwhelmed, but Olivo says these concerns have mostly faded as the program has grown.
Olivo finds it therapeutic to know that fewer children in Rifle now have to interpret for their parents at the hospital. She feels a sense of healing, knowing that teenagers can be "let off the hook" and their parents will be taken care of.
Olivo and Dr. Coleman hope to expand the program further by hiring dedicated interpreters in departments that need them most.