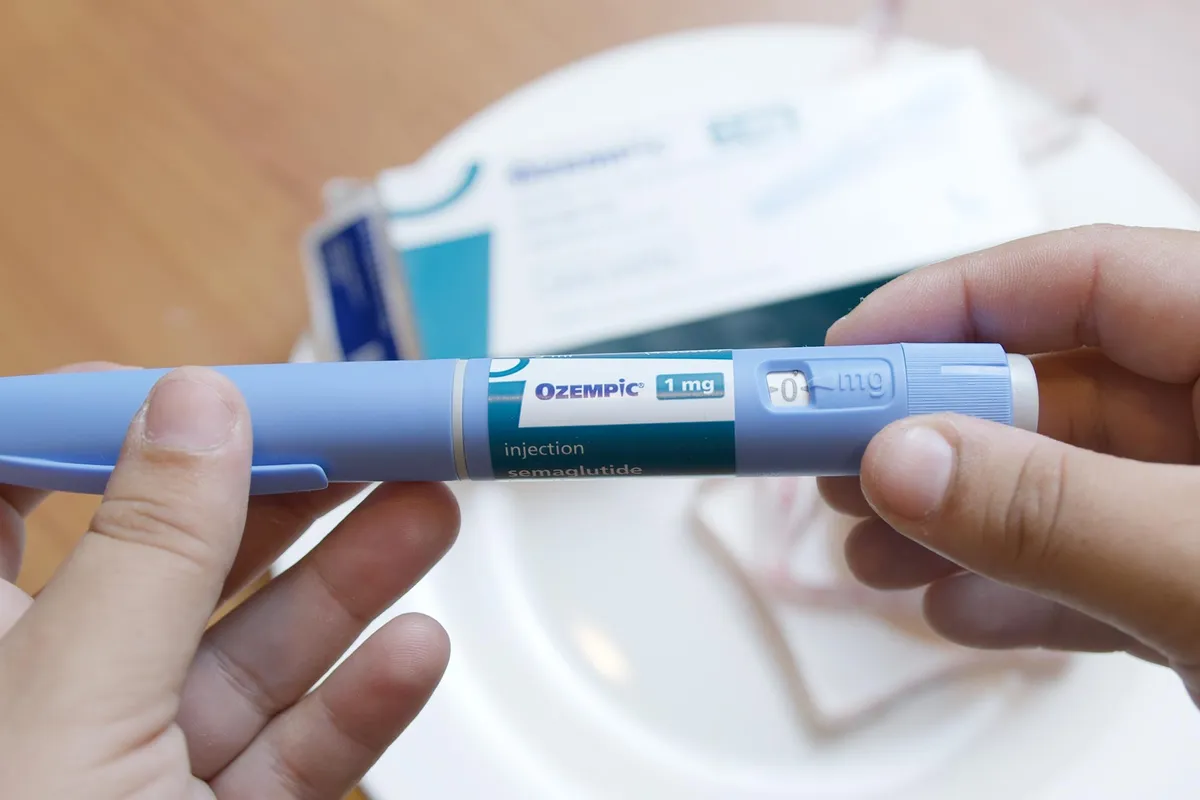
Around 1.5 million people in the UK are taking GLP-1 medications like Ozempic and Wegovy. Most got them from private clinics with little more than a prescription. That's a problem, according to researchers from UCL and Cambridge — because these drugs do something most people don't realize: they can reshape what your body actually loses.
When semaglutide or tirzepatide work on your appetite, they work well. People taking them eat 16 to 39 percent less food. The weight comes off. But here's what gets overlooked: up to 40 percent of that lost weight can be muscle, not fat. Lose the wrong kind of weight fast enough, and you're trading one health problem for another.
The gap between the drug and the support
Dr. Adrian Brown from UCL's Centre of Obesity Research puts it plainly: "Without appropriate nutritional guidance, there is a real risk that reduced food intake could compromise dietary quality, meaning people may not get enough protein, fibre, vitamins, and minerals essential for maintaining overall health."
We're a new kind of news feed.
Regular news is designed to drain you. We're a non-profit built to restore you. Every story we publish is scored for impact, progress, and hope.
Start Your News DetoxThe evidence backing this concern is thin — researchers found just 12 studies examining nutrition alongside these medications. But the logic is sound. When appetite suppression is this powerful, what you eat matters more than ever. Grab whatever feels tolerable when nausea hits, and you might hit your calorie target while missing essential micronutrients. Protein intake drops. Muscle loss accelerates. Fatigue, weakened immunity, and hair loss follow.
The irony is that NHS guidance explicitly recommends these drugs only as part of a wider program including dietary support and physical activity. In practice, 95 percent of UK users access them privately, where that structured support often doesn't exist.
What we can learn from surgery
Researchers point to gastric bypass and banding surgery as a model. Those procedures have been around longer, and the post-operative nutritional protocols are well-established: prioritize protein across small, frequent meals; focus on nutrient-dense foods; monitor micronutrient levels. The weight loss mechanism is similar to GLP-1 drugs, so the lessons transfer.
Dr. Marie Spreckley from Cambridge's MRC Epidemiology Unit notes that "use of GLP-1 receptor agonist therapies has increased rapidly in a very short period of time, but the nutritional support available to people using these medications has not kept pace." The team is launching AMPLIFY, a research project that will directly ask people using these drugs what support they actually need — particularly people from communities historically underrepresented in obesity research.
The medications themselves aren't the problem. They're transforming obesity care. But the gap between what the drugs do and what people are told to eat is real, and it's preventable. That gap is closing — just not fast enough yet.