A 33-year-old man walked out of the hospital more than two years later with fully functioning lungs—after his own were surgically removed and replaced with a machine.
He'd arrived with the flu. It turned into bacterial pneumonia. His lungs filled with inflammation so severe they stopped working entirely, and the infection began shutting down his heart and kidneys too. Doctors faced an impossible choice: his lungs were too damaged to recover, but his body was too unstable to survive transplant surgery.
So they removed both lungs and connected him to an artificial lung system—essentially a machine that did what his lungs couldn't. It pulled oxygen into his blood, pushed carbon dioxide out, and kept his circulation steady enough for his heart to keep beating. For 48 hours, this device was his entire respiratory system.
We're a new kind of news feed.
Regular news is designed to drain you. We're a non-profit built to restore you. Every story we publish is scored for impact, progress, and hope.
Start Your News Detox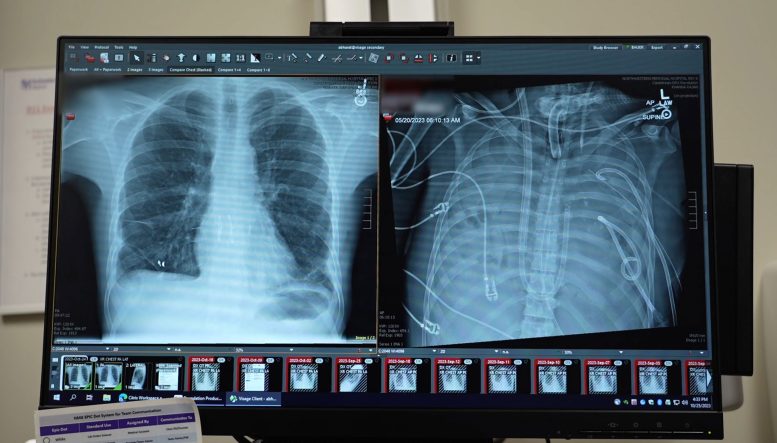
The Bridge That Bought Time
Without his damaged lungs driving infection through his body, something shifted. His blood pressure stabilized. His other organs began working again. The infection came under control. Two days into the artificial lung support, compatible donor lungs became available, and surgeons performed the transplant.
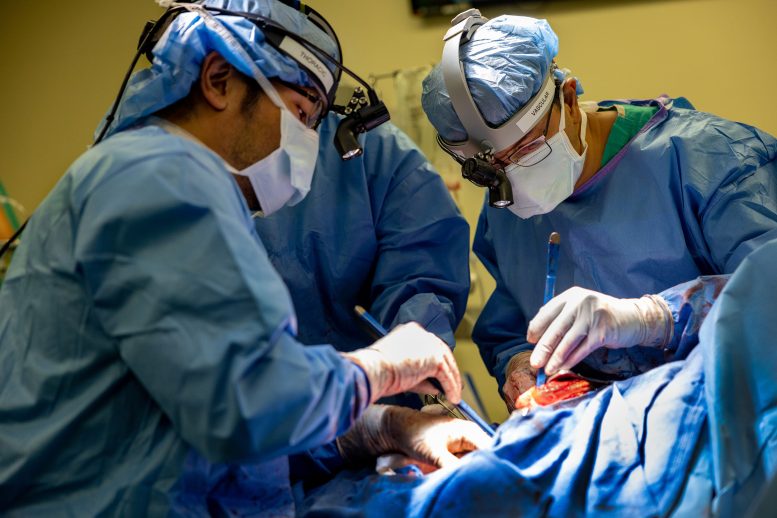
"The heart and lungs are intrinsically connected," says Dr. Ankit Bharat, who led the procedure. "When there are no lungs, how do you keep the patient alive?" The answer, it turned out, was engineering.
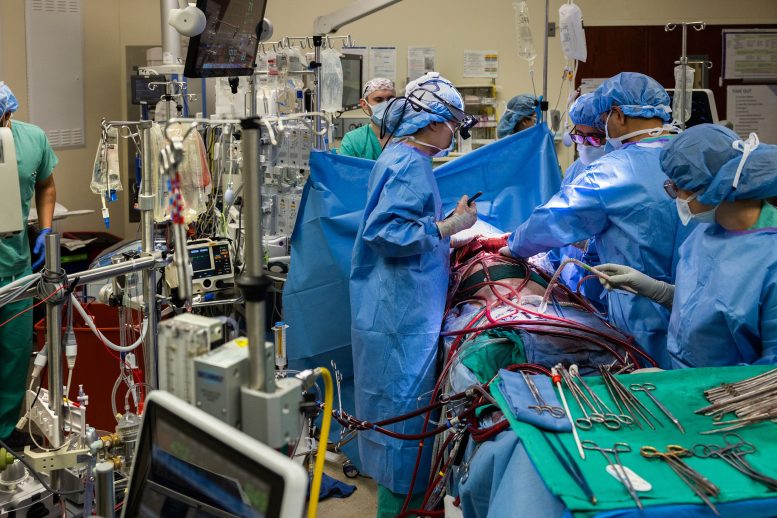
What makes this case significant isn't just that it worked. It's what the removed lungs revealed. Molecular testing showed extensive scarring and immune damage so severe the tissue would never have healed on its own. This is the first biological proof that some patients with severe ARDS—acute respiratory distress syndrome—need transplants to survive, not just time and support.
"For the first time, biologically, we are giving molecular proof that some patients will need a double lung transplant; otherwise, they will not survive," Bharat says.
Right now, only a handful of specialized hospitals can perform this procedure. Young patients with catastrophic lung damage from viruses or infections die regularly because no one considered transplant an option. Bharat is working to standardize the artificial lung technology so more hospitals can access it, and more importantly, so doctors recognize earlier when transplant is the lifesaving choice.

The next frontier isn't just keeping patients alive on machines—it's knowing when to move forward with transplant before irreversible damage takes hold.