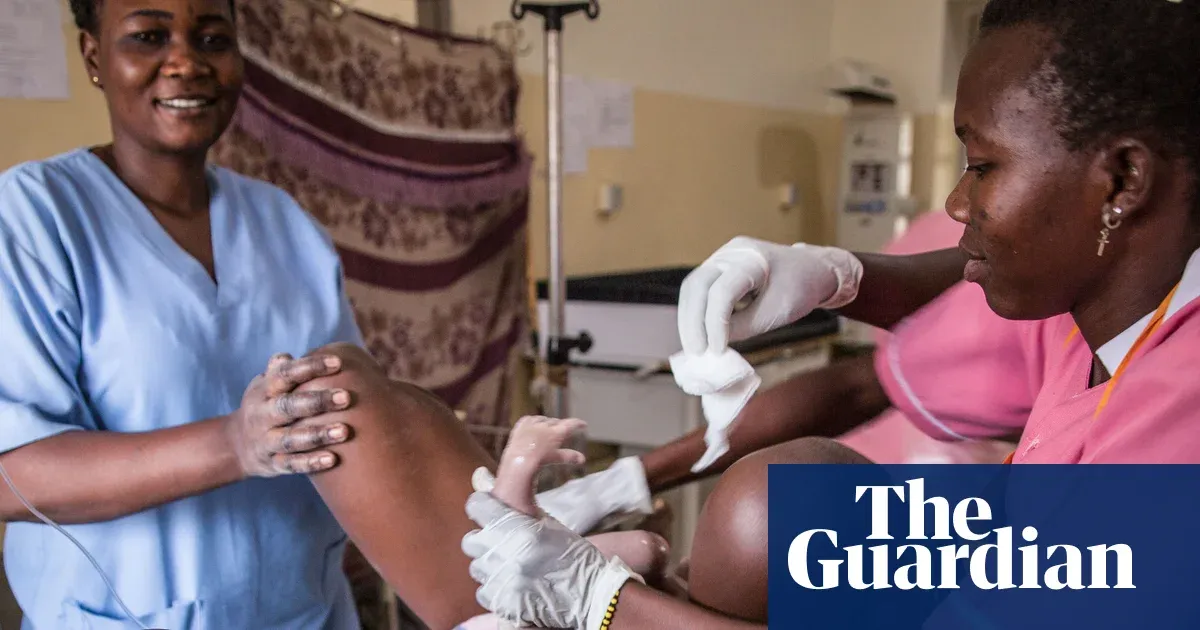
A gap of nearly 1 million midwives is forcing pregnant women into unnecessary medical interventions and leaving health systems unable to prevent deaths that could be avoided.
The shortage is not evenly distributed. Africa carries nearly half the global deficit, with 9 in 10 women there living in countries without adequate midwife coverage. The eastern Mediterranean region has only 31% of the midwives it needs; the Americas, 15%. Even in better-resourced regions like Europe and Southeast Asia, gaps persist.
When midwives are scarce, what happens in the delivery room changes. Hospitals become bottlenecks. Care becomes rushed. Women experience more caesarean sections, more inductions, more interventions — not always because they're medically necessary, but because stretched systems default to procedures that move women through faster. Anna af Ugglas, CEO of the International Confederation of Midwives, frames it plainly: "Intervention rates rise, and women are more likely to experience poor-quality care or mistreatment."
We're a new kind of news feed.
Regular news is designed to drain you. We're a non-profit built to restore you. Every story we publish is scored for impact, progress, and hope.
Start Your News DetoxWhat Full Staffing Could Actually Do
The math is striking. If 980,000 additional midwives were trained and deployed across 181 countries, universal access to midwife-led care could prevent two-thirds of maternal deaths, newborn deaths, and stillbirths. That's 4.3 million lives saved annually by 2035.
But the problem isn't only training. Countries train midwives and then don't hire them. Or they hire them and pay them so poorly that experienced midwives leave for other work. The issue is investment and retention, not just pipeline.
The International Confederation of Midwives is pushing governments to act — not with vague commitments, but with concrete funding and employment guarantees. The political will exists in pockets: some countries are expanding midwifery education and creating stable career paths. Others are still treating it as an afterthought.
What's becoming clearer is that maternal safety isn't just a medical question. It's a workforce question. And workforce questions require the kind of sustained funding that usually gets outcompeted by more visible health emergencies. The gap won't close by accident.