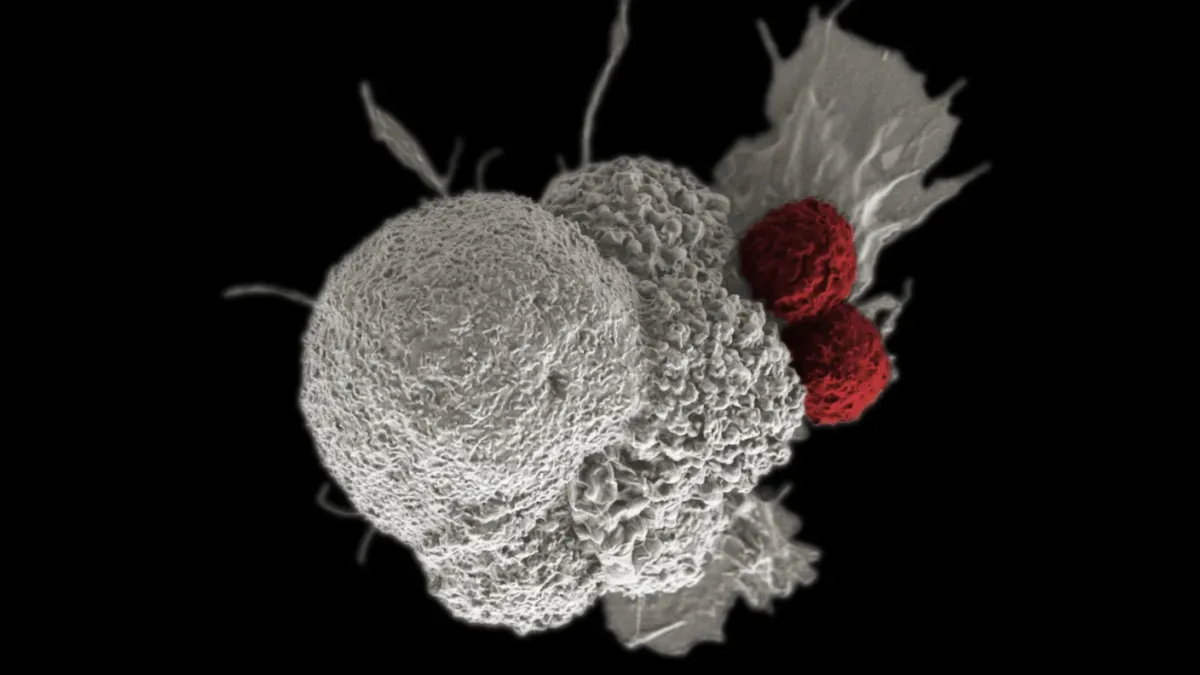
A small trial is testing whether cancer cells, stripped of their ability to grow, can teach the body to recognize and attack real tumors.
The approach sounds counterintuitive: take cancer cells from a patient, disable them, then put them back in. But PhotonPharma, a company founded by Colorado State University researcher Ray Goodrich, is now running the first human test of this idea. The logic is straightforward. Disabled cancer cells retain their distinctive protein signals—the markers that make them look like cancer. Reintroduced into the body, they could act like a wanted poster, helping the immune system identify and eliminate the actual tumor.
How an old blood-safety technique became a cancer treatment
The method, called the Mirasol process, wasn't originally designed for cancer at all. In the late 1980s, during the HIV epidemic, Goodrich was working to purify donated blood. Contamination was a critical problem. After a decade of experimentation, he found an elegant solution: vitamin B2 (riboflavin) combined with ultraviolet light. The riboflavin binds to DNA and RNA, and the UV blast damages genetic material in pathogens, stopping them from reproducing. The blood stayed intact; the threats were neutralized.
We're a new kind of news feed.
Regular news is designed to drain you. We're a non-profit built to restore you. Every story we publish is scored for impact, progress, and hope.
Start Your News DetoxThen Goodrich noticed something unexpected. Some white blood cells survived the process—their structure remained whole, but they could no longer divide or function. They were, in effect, zombies. The observation sparked a question: could cancer cells be disabled the same way and used to train the immune system.
It took years of research in animals to test the idea. Mice and dogs with recurrent cancers showed promise when treated with these disabled tumor cells. That track record convinced Goodrich to launch PhotonPharma and move toward human trials.
The first test
The current trial focuses on people with advanced, recurrent ovarian cancer who have exhausted other treatment options. Researchers will remove cancer cells from each patient, inactivate them using UV light and riboflavin, then add molecules commonly used in vaccines to amplify the immune response. Participants will receive three doses of their own disabled cancer cells while the team monitors for side effects and tracks immune activity.
Success isn't assured. Tumors are skilled at suppressing immune attacks, and it's unclear whether UV-treated cells can restore that immune vigor. Goodrich himself is measured about the potential. "You would always hope, but I think it's too optimistic to think that it completely cures it," he told The Colorado Sun. "But it's maybe something that could add years of life, of good-quality life, onto someone's lifespan."
For patients with few alternatives, adding years of good quality matters. If early results hold, the team plans to expand the trial and test the approach on other solid tumors. The path from a blood-safety discovery to a cancer vaccine shows how unexpected observations—a scientist noticing zombie cells—can reshape how we think about disease.