A seven-year-old boy lies in a Malawi hospital receiving treatment for polio—a disease the country hadn't seen in three years. Within days of detecting the virus in sewage samples from Blantyre, the country's second-largest city, health workers had vaccinated 1.3 million children in just four days. Emergency vaccine supplies arrived by plane from the World Health Organization, and the campaign moved fast.
Polio is a virus that spreads silently. Most people experience only mild symptoms, yet it causes permanent paralysis or death in a small but significant percentage of cases, especially in children. A single case is considered dangerous, particularly in areas where vaccination rates are low. This outbreak—detected through environmental sampling before any widespread transmission—is a reminder of how fragile progress can be. Twenty-eight years ago, the world had reduced polio cases from millions to just 2,880 in 20 countries. But the virus has proven stubbornly persistent in remote regions with weak health infrastructure.

The Trust Problem
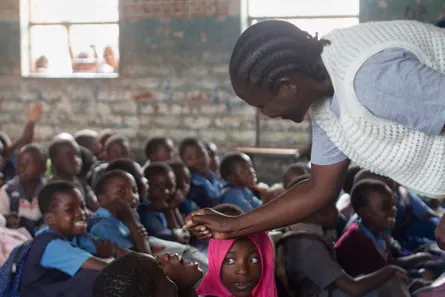
The real battle isn't just against the virus—it's for the trust of communities where vaccination rates remain low. In Ndirande township, health workers visited nurseries, schools, and homes. Some mothers had never heard of polio. Others were hesitant. One 21-year-old mother said she didn't know much about the vaccine and felt her four-year-old had "had enough vaccines in her life." At a primary school, about one in ten children sat at their desks while others lined up for the vaccine—their parents had withheld permission for religious or personal reasons.
We're a new kind of news feed.
Regular news is designed to drain you. We're a non-profit built to restore you. Every story we publish is scored for impact, progress, and hope.
Start Your News DetoxBut something shifted when local leaders got involved. Community health workers, religious leaders, and traditional authorities began correcting misinformation and reassuring families. In Ndirande, 45 of 84 initially reluctant households accepted vaccination after this targeted engagement. Sheeba Afghani, a senior manager with Unicef's polio programme, has witnessed this dynamic across multiple countries. "You can give her any argument," she says of vaccine-hesitant mothers. "It doesn't matter. And then you have a local influencer walk in, and he says 'vaccinate', and she just hands you the child."
Local trust matters more than scientific argument—a lesson polio workers have learned repeatedly in Afghanistan and Pakistan, where the wild virus remains endemic.


Misinformation at Scale
Then came social media. Once, if a false rumor about vaccination deaths circulated, community leaders and doctors would arrive locally within days to address it. "Now, even before we've had the opportunity to arrive in the community, it'll be on social media," Afghani says. The phrase "vaccine-derived" itself creates innocent confusion—it sounds like you get polio from the vaccine, which is false. High-profile voices casting doubt on vaccination programs amplify this confusion. When uncertainty spreads, rumors flourish.
In 2019, staged videos of children allegedly collapsing after polio vaccination in Pakistan forced a programme suspension. The panic led to health clinics being set on fire, thousands of children rushed to hospitals by panicked parents, and the deaths of a health worker and two police officers.

Afghanistan presents a different crisis. Half of last year's recorded wild polio cases occurred there, yet the Taliban's restrictions on women working and girls attending school have locked mothers behind closed doors—unreachable by vaccination teams. Outreach drives have become impossible.

The Funding Squeeze

Money is drying up at a critical moment. The Global Polio Eradication Initiative saw funding fall last year as major donors including the US and Britain cut aid spending. With a $1.7 billion funding shortfall in its 2022-29 strategy, the initiative warned it would no longer respond "at scale" to all outbreaks as it did in Malawi this month.
Malawi itself is particularly vulnerable. Fifty-five percent of its total health expenditure comes from donors, and massive aid cuts are hitting hard. Dr Mike Chisema, Malawi's Ministry of Health immunisation programme manager, describes the impact: "The funding space has really shrunk, and this has affected a lot of services." Yet he remains committed. "While the funds may not be adequate, there is always something to push the countries to respond."
Malawi now tests weekly in some places and fortnightly in others, actively hunting for cases and encouraging community reporting. Ruth Kutaombe, holding her eight-month-old boy at a health centre in Ndirande, chose vaccination after hearing about it at a routine clinic visit. "It will protect him from contracting the disease," she says.



Unicef teams are experimenting with "microinfluencers" who challenge misinformation online and maintain a dashboard at their New York headquarters that scours social media for polio mentions. Any spike suggesting rumors are spreading before a planned campaign can be met with swift response. The strategy acknowledges what Afghani has learned: boycotts are often led by people who support vaccination but feel conflicted. Their first loyalty is to their community, which faces bigger challenges than disease prevention alone.
Polio eradication has always been a race against time and skepticism. Malawi's response—rapid vaccination, community engagement, and persistent surveillance—offers a model for how to move fast without leaving people behind.