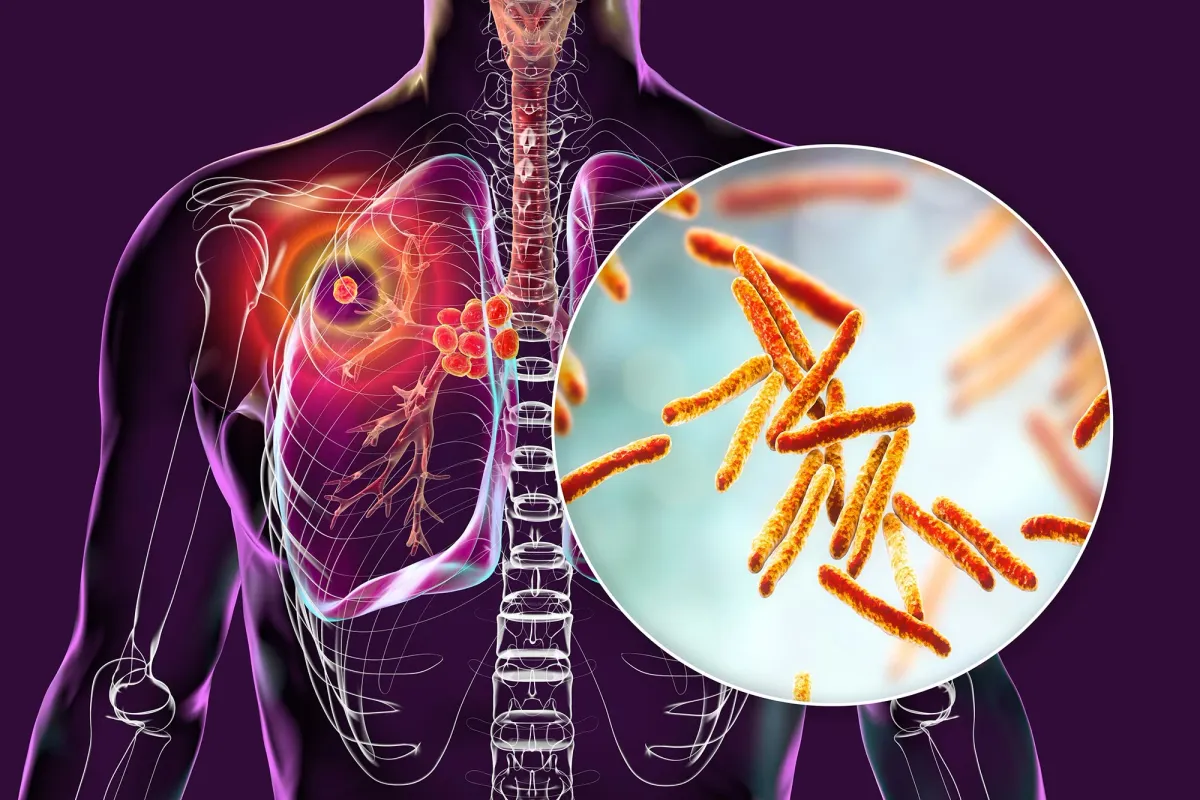
Tuberculosis treatment has a stubborn problem: the drugs that work best often come with a catch. Rifampin, one of the most effective TB medications, has to be taken by mouth every single day for months. It damages the liver. And here's the frustrating part—most of it never reaches the lungs, where TB bacteria actually hide.
Researchers at the University at Buffalo just published a study showing a way around this. They've engineered microscopic nanoparticles that carry rifampin directly into the lungs when you breathe them in. In mouse models, a single weekly inhalation kept drug levels in lung tissue high for up to seven days—something daily pills couldn't match.
How the particles work
Think of these nanoparticles as tiny delivery trucks with a specific destination. Each one has a biodegradable core loaded with rifampin. The outer layer is coated with a naturally derived molecule designed to be recognized and absorbed by macrophages—the immune cells that TB bacteria infect and hide inside. This dual design means the drug gets to exactly where it needs to be, and stays there longer.
We're a new kind of news feed.
Regular news is designed to drain you. We're a non-profit built to restore you. Every story we publish is scored for impact, progress, and hope.
Start Your News Detox"These particles are specially built to go straight to the lungs and be taken up by the immune cells where TB bacteria hide," explains Hilliard Kutscher, the study's first author. "They slowly release the drug over time, stimulate the immune system to fight TB better, and reduce exposure to the rest of your body."
That last part matters. Because rifampin stays in the lungs instead of circulating through your whole system, patients experience fewer side effects—particularly liver damage, which is a real concern with daily oral doses.
The research team tested their approach in two separate mouse models of TB, comparing weekly inhaled nanoparticle therapy against the standard daily oral rifampin. The inhaled version kept higher drug concentrations in lung tissue for much longer. The implication is significant: patients might eventually need treatment only once a week instead of taking a pill every morning for six months or more.
Why this shifts something real
TB treatment adherence is already a global problem. Six months of daily pills is a long commitment, especially for people managing poverty, unstable housing, or competing health crises. Miss doses, and the bacteria develop resistance. A weekly treatment—delivered in a way that reduces side effects—could change the math for millions of people, particularly in regions where TB burden is highest.
Jessica Reynolds, the study's senior author, notes that "reducing treatment frequency could improve adherence, lower side effects, and make TB care more accessible worldwide." That's not hyperbole. It's the practical reality of how treatment schedules affect real outcomes.
The researchers also see potential beyond TB itself. Rifampin is used to treat other serious lung infections caused by non-tuberculous mycobacteria, which are becoming more common in the U.S. Delivering the drug directly to infected tissue while minimizing bloodstream exposure could reduce harmful drug interactions and allow more effective treatment across a broader range of pulmonary infections.
The next phase involves testing whether these nanoparticles can be combined with other standard TB antibiotics. TB treatment has always relied on combination therapy—multiple drugs working together to prevent resistance. If this approach works with the full drug regimen, it could genuinely reshape how TB is treated globally.