Grace Bell was 16 when a doctor told her she wouldn't carry her own child. She has MRKH syndrome, a condition that affects around 5,000 women in the UK—she was born without a womb, though her ovaries work normally. For years, that felt final. Then, in June 2024, she received a phone call that changed everything: a womb was available for transplant.
Hugo arrived just before Christmas 2025, weighing nearly 7 pounds. He is the first baby in the UK born to a mother who received a womb from a deceased donor—a milestone that opens a new path for thousands of women who were told motherhood wasn't possible for them.
From Shock to Surgery
When Bell learned a transplant was possible, she was "in complete shock and really excited." But she was acutely aware of what the donor family had given up. "I think of my donor and her family every day," Bell said, "and pray they find some peace in knowing their daughter gave me the biggest gift: the gift of life."
We're a new kind of news feed.
Regular news is designed to drain you. We're a non-profit built to restore you. Every story we publish is scored for impact, progress, and hope.
Start Your News DetoxThe transplant operation itself lasted 10 hours at The Churchill Hospital in Oxford. Months later, Bell and her partner Steve Powell underwent IVF treatment, followed by embryo transfer at The Lister Fertility Clinic in London. The pregnancy progressed, and Hugo was born at Queen Charlotte's and Chelsea Hospital in west London.
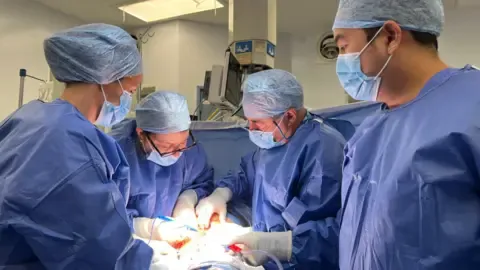
Bell remembers the moment she saw him: "It was simply a miracle. I remember waking up in the morning and seeing his little face, with his little dummy in, and it felt like I needed to wake up from a dream."
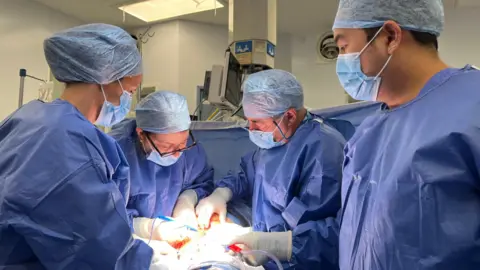
A Rare Achievement, Globally
Hugo's birth is one of only a handful in Europe resulting from a deceased donor womb transplant. Globally, more than 100 womb transplant operations have been performed, with over 70 healthy babies born as a result. The UK trial, of which Bell's case is part, aims to establish whether this procedure could become a standard treatment option.
Consultant gynaecologist Prof Richard Smith from Imperial College Healthcare NHS Trust, who has researched womb transplantation for over 25 years and was present at Hugo's birth, emphasized the scale of coordination required. "A huge team of people" worked across transplant surgery, embryo transfer, and delivery. The couple honored Smith's role by giving Hugo the middle name Richard.
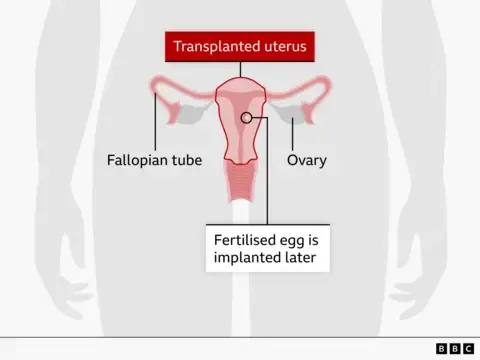
Transplant surgeon Isabel Quiroga called the birth a breakthrough for organ transplantation in the UK. "Very few babies have been born in Europe as a result of their mothers receiving a womb from a deceased donor," she said. "Our trial is seeking to discover whether this procedure could become an approved and regular treatment."
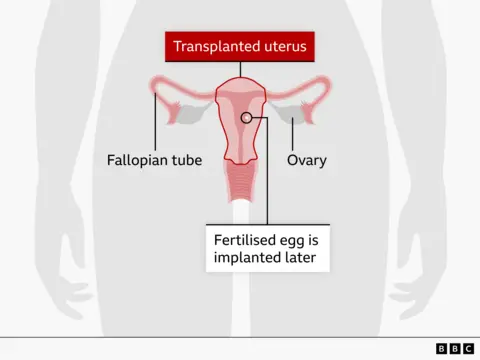
What Comes Next
Bell and Powell may choose to have a second child. After that, surgeons will remove the transplanted womb—a choice that spares Bell from taking immunosuppressant drugs for life. The donor's family, who wish to remain anonymous, said they felt "tremendous pride" at their daughter's legacy. Beyond the womb, she donated five other organs, which were transplanted into four people.
For girls and young women told they had no viable womb, Smith said the message is now different: hope is possible. Hugo's arrival signals that the conversation has shifted from "you can't" to "here's how you might."










