For people with Parkinson's disease, deep brain stimulation has been transformative—but it doesn't work equally well for everyone. A new study suggests why: researchers have identified a specific brain rhythm that appears to determine how much a patient will benefit from the treatment.
Parkinson's affects movement control, making everyday actions slower, stiffer, or shakier. Deep brain stimulation (DBS) sends small electrical pulses into the subthalamic nucleus, a deep brain region involved in movement, and it's one of the most effective treatments available. Yet some patients experience dramatic improvement while others see modest gains. Until now, nobody fully understood why.
Scientists from universities in Cologne, Düsseldorf, and Berlin—working with Harvard Medical School—analyzed data from 50 patients (100 brain hemispheres) who had DBS implants. Using both the electrical signals recorded directly from the implanted electrodes and a brain imaging technique called magnetoencephalography (MEG), they mapped how the deep brain regions communicate with the cortex (the brain's outer layer).
We're a new kind of news feed.
Regular news is designed to drain you. We're a non-profit built to restore you. Every story we publish is scored for impact, progress, and hope.
Start Your News Detox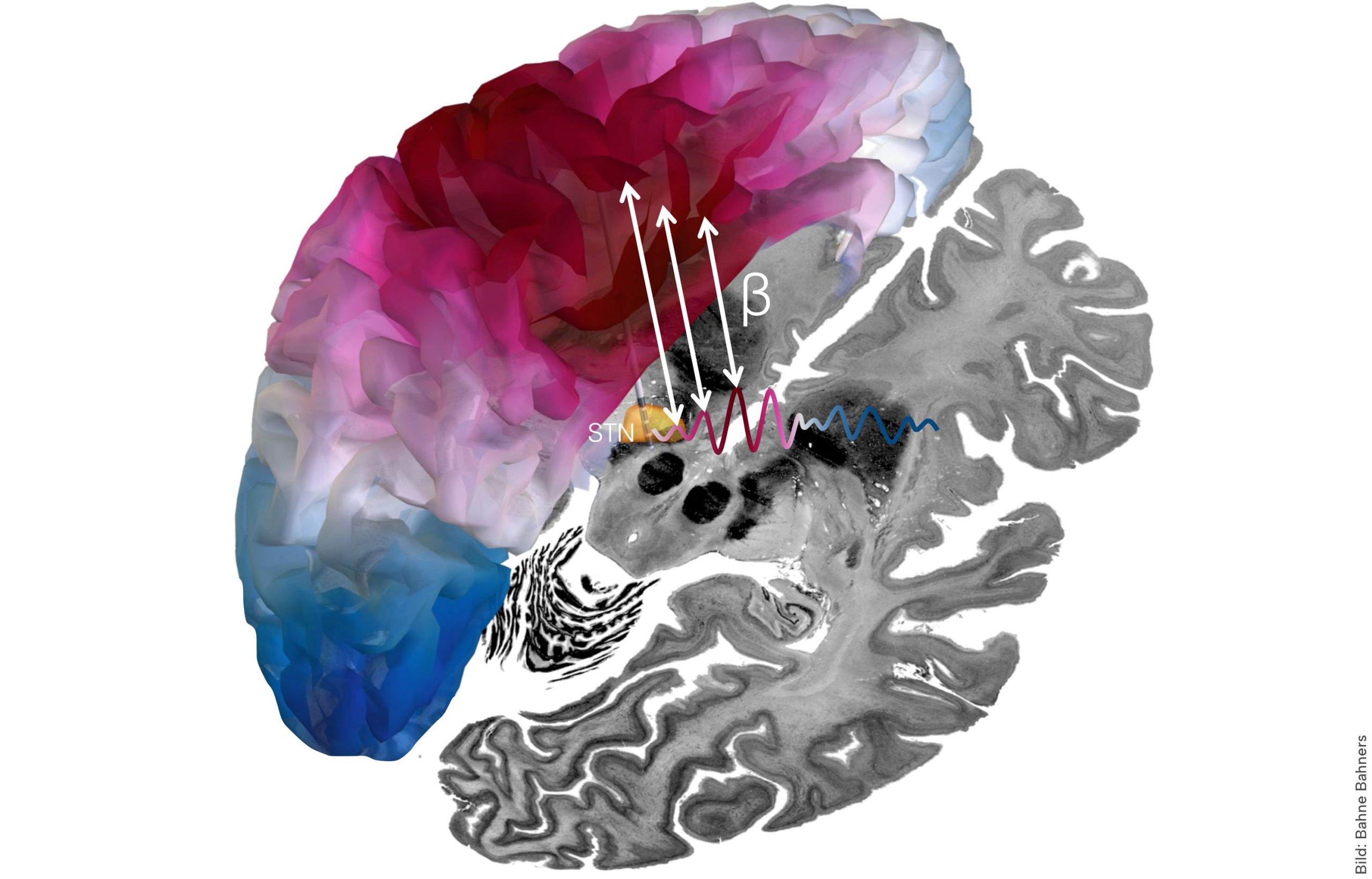
The Rhythm That Matters
The key finding: the brain regions involved in movement control communicate most strongly at a specific frequency—the "beta" range of 20 to 35 Hz (cycles per second). This rhythm has long been suspected to play a role in Parkinson's symptoms; abnormal beta patterns are linked to the slowed movement characteristic of the disease. What's new is showing that the strength of this communication directly correlates with how well a patient responds to DBS.
Professor Andreas Horn, who led the research, describes it as the first time scientists have mapped both the location and timing of the effective DBS network simultaneously. "We show that Parkinson's disease can best be treated if we stimulate a very precisely defined network," he explains. "This network operates synchronized within a specific frequency band."
The practical implication is significant. Right now, doctors adjust DBS settings somewhat empirically—trial and adjustment based on what works for each patient. This discovery suggests a more precise path forward. "By stimulating regions that are connected to the identified network, we will probably be able to adjust DBS settings more precisely in the future, especially in patients who have not yet benefited optimally," notes Dr Bahne Bahners, the study's first author.
The research team is already planning the next phase: studying the causal relationship between DBS and these brain networks. If they can confirm that stimulating the right parts of this network directly improves symptoms, it could reshape how the treatment is personalized—potentially unlocking better outcomes for patients who currently see only partial benefit.
Study Title - Brain, 2026