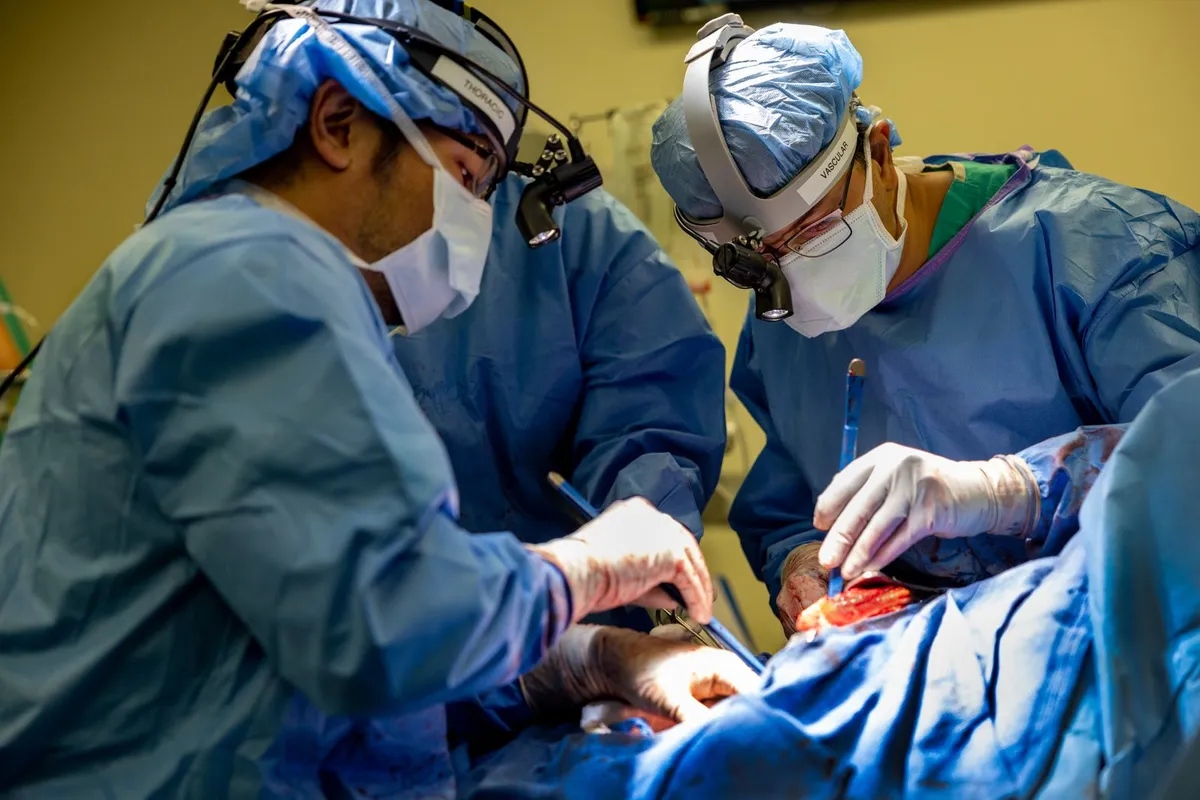
A 33-year-old man arrived at Northwestern Memorial Hospital in Chicago in spring 2023 barely clinging to life. Flu had triggered a cascade of complications—fluid was pooling in his lungs, a bacterial infection was taking hold, his kidneys were shutting down, and his heart had stopped. His doctors performed CPR, but as thoracic surgeon Ankit Bharat recalls, "it was very clear that we had to do something right away."
They faced an impossible choice: his diseased lungs were fueling the infection, but he was too fragile to survive transplant surgery. So they made a radical decision. They removed his lungs entirely and replaced them with an artificial system—essentially a mechanical bridge to keep him alive long enough to become a transplant candidate.
The device works by pulling blood directly from the right side of the heart, infusing it with oxygen, and pumping it back to the left side to circulate through his body. Within 48 hours, the transformation was striking. "He was off all the medication to support his blood pressure, his kidney function was completely restored and his heart was working normally," Bharat says. The patient recovered enough to receive a double lung transplant. Nearly three years later, he's doing well.
We're a new kind of news feed.
Regular news is designed to drain you. We're a non-profit built to restore you. Every story we publish is scored for impact, progress, and hope.
Start Your News DetoxA new kind of life support
What makes this breakthrough significant isn't just that it worked once—it's what it reveals about severe lung failure. Doctors have long assumed that critically ill patients with acute respiratory distress syndrome (ARDS) simply need time and support; eventually, the thinking went, the lungs would heal themselves. But when Bharat's team analyzed this patient's lungs after removal, they discovered damage so severe the organs could never have recovered on their own.
"For the first time, biologically, we are giving molecular proof that some patients will need a double lung transplant, otherwise they will not survive," Bharat explains. That's not just a clinical observation—it's a shift in how doctors might approach the most desperate cases.
The artificial lung system itself builds on existing technology called ECMO (extracorporeal membrane oxygenation), which has been used for years to handle gas exchange in critical patients. But this upgraded version does something ECMO cannot: it also manages blood flow to and from the heart itself, making it a more complete replacement for lung function.
Bharat emphasizes that there's nothing proprietary about the design. "There is nothing proprietary about this," he says. "Anybody can replicate that." Northwestern is now offering the system to patients who are running out of time, while maintaining a registry to track outcomes and refine the approach.
The question now is whether this "nuclear option"—as Bharat calls it—becomes a tool other hospitals can deploy, and whether it changes how we think about which patients might still be saved.