Researchers have found that measuring how well blood moves through your brain could reveal Alzheimer's risk before memory problems start — using tools so simple they work while you're sitting quietly.
The discovery, from USC's neuroimaging institute, suggests that the health of your brain's blood vessels matters as much as the protein tangles we've long blamed for cognitive decline. When blood flows efficiently and oxygen reaches brain tissue properly, people tend to have fewer amyloid plaques (the hallmark protein buildup in Alzheimer's) and larger hippocampi — the memory centers that typically shrink with the disease.
"Amyloid and tau get all the attention, but blood flow and oxygen delivery are also critical," says Amaryllis Tsiknia, the lead researcher. "When the brain's vascular system functions like it does in healthy aging, we see brain features linked to better cognitive health."
We're a new kind of news feed.
Regular news is designed to drain you. We're a non-profit built to restore you. Every story we publish is scored for impact, progress, and hope.
Start Your News DetoxHow They're Measuring It
The team used two techniques that require nothing invasive. Transcranial Doppler ultrasound measures blood speed through major brain arteries — the same technology used in routine pregnancy scans. Near-infrared spectroscopy estimates how effectively oxygen reaches tissue near the brain's surface. Combined with advanced math modeling, these readings show how well the brain regulates its own blood supply when blood pressure or carbon dioxide levels shift.
People with healthier vascular function scores had lower amyloid accumulation and larger hippocampal volumes. Those diagnosed with mild cognitive impairment or dementia showed weaker vascular function across the board — suggesting reduced blood flow is part of the disease spectrum, not just a side effect.
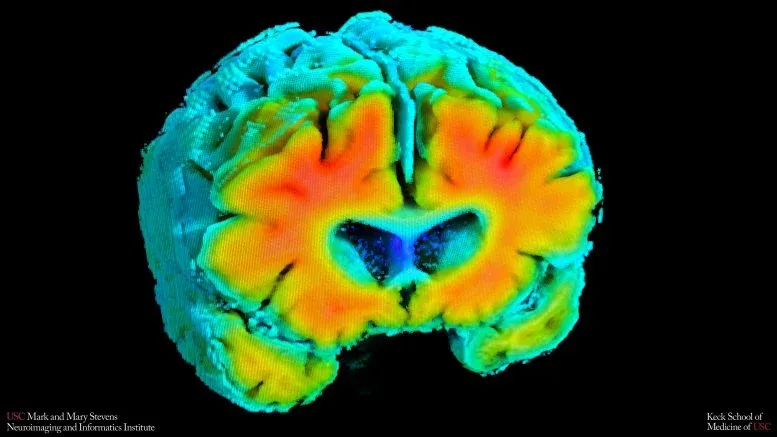
Why This Changes the Game
Here's what makes this genuinely useful: MRI and PET scans are expensive, time-consuming, and sometimes inaccessible. They require injections, radiation, or complex tasks. These vascular measures don't. That means they could screen far more people, far more cheaply — catching risk before it becomes crisis.
But there's a deeper insight here. For decades, Alzheimer's research has treated the disease as primarily a protein problem: amyloid plaques and tau tangles accumulate, neurons die, memory fades. This study suggests that framing is incomplete. Your brain's plumbing matters. If blood can't deliver oxygen efficiently, neurons suffer — whether or not plaques are present. It's the difference between blaming the poison and ignoring the fact that the patient isn't breathing well.
This also explains why some interventions (exercise, Mediterranean diet, cognitive engagement) seem to help with dementia risk even though they don't directly clear plaques. They improve cardiovascular health, which improves brain blood flow.
The researchers are careful to note this is a snapshot, not proof of cause and effect. Ongoing studies will track whether vascular measures actually predict future cognitive decline and whether improving blood flow can slow brain changes. But the foundation is laid.
"If we can track these signals over time, we may identify people at higher risk earlier and test whether improving vascular health can slow Alzheimer's-related brain changes," Tsiknia says.
The next phase is clear: long-term follow-up studies to see if these vascular measures can forecast who'll decline and whether interventions targeting blood flow actually work. If they do, the screening landscape for dementia risk could shift dramatically — from expensive, specialized imaging to simple, accessible tests that work in any clinic.