A team at Scripps Research just figured out something quietly elegant: the shape of proteins in your blood might tell you more about Alzheimer's than their quantity ever could.
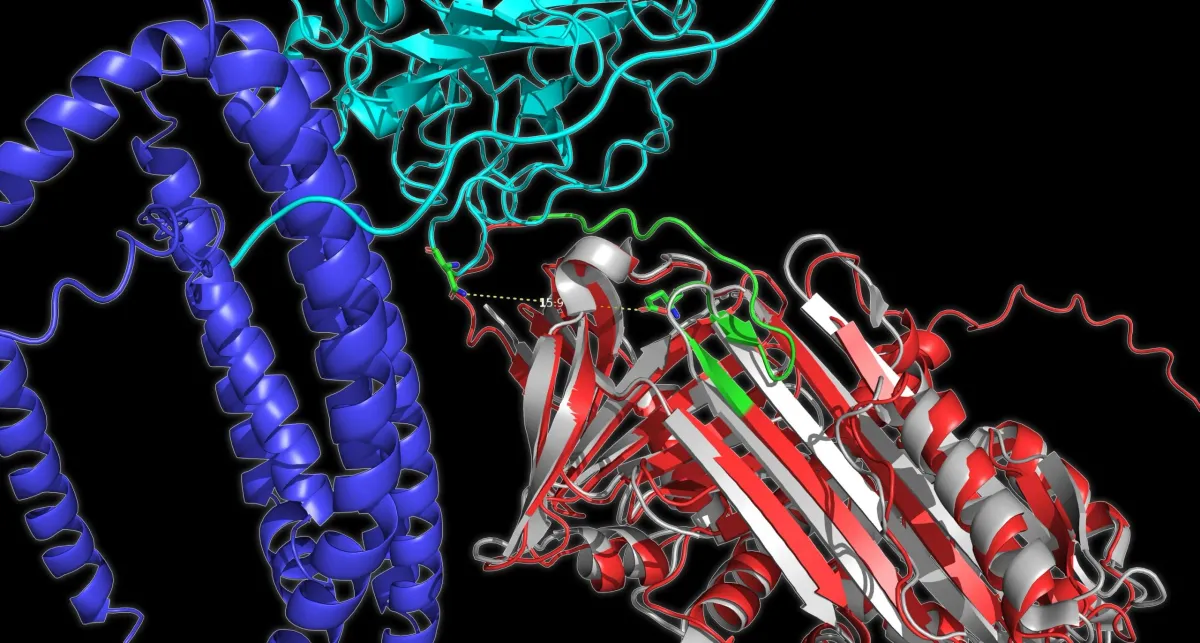
For years, doctors have looked for Alzheimer's by measuring how much amyloid beta and tau protein show up in blood tests. But a new study published in Nature Aging suggests that's only half the story. What actually matters is how those proteins are folded—whether they're tightly wrapped or loosely unraveled. That structural difference appears early, possibly before the cognitive decline that defines the disease.
Alzheimer's affects about 7.2 million Americans over 65. The disease develops quietly for years before symptoms hit. Earlier detection means earlier treatment, and early treatment, the research suggests, could make a real difference in preserving memory.
We're a new kind of news feed.
Regular news is designed to drain you. We're a non-profit built to restore you. Every story we publish is scored for impact, progress, and hope.
Start Your News DetoxWhy protein shape matters
Your cells have a quality-control system that keeps proteins folded correctly and clears out the damaged ones. It's called proteostasis, and it's basically the cellular equivalent of a dishwasher—it keeps things clean and organized. As you age, this system gets tired. Proteins start to fold wrong. The brain suffers first, but here's the insight: if something's going wrong in your brain, signs of it should show up in your blood too.
The researchers tested this theory on 520 people—some with normal cognition, some with mild memory problems, some with full Alzheimer's. Using mass spectrometry (a technique that can read the atomic structure of molecules), they mapped which parts of specific blood proteins were exposed or buried, looking for signs of misfolding.
Three proteins stood out: C1QA, which helps coordinate immune responses; clusterin, which clears out damaged proteins; and apolipoprotein B, which transports fats. Changes at specific sites within these proteins let the team classify people into disease categories with about 83% accuracy overall. When separating healthy people from those with early memory loss, they hit 93% accuracy.
"It was very surprising to find three lysine sites on three different proteins that correlate so highly with disease state," said Casimir Bamberger, a senior scientist on the team. The researchers tested the same people again months later, and the protein panel held up, correctly identifying disease status about 86% of the time.
What happens next
Before this becomes a standard clinical test, larger studies with longer follow-ups will be needed. But the team is already exploring whether the same approach works for Parkinson's disease and cancer.
The real promise here is timing. If you can catch structural changes in blood proteins before brain damage gets serious, treatment has a fighting chance to actually work.