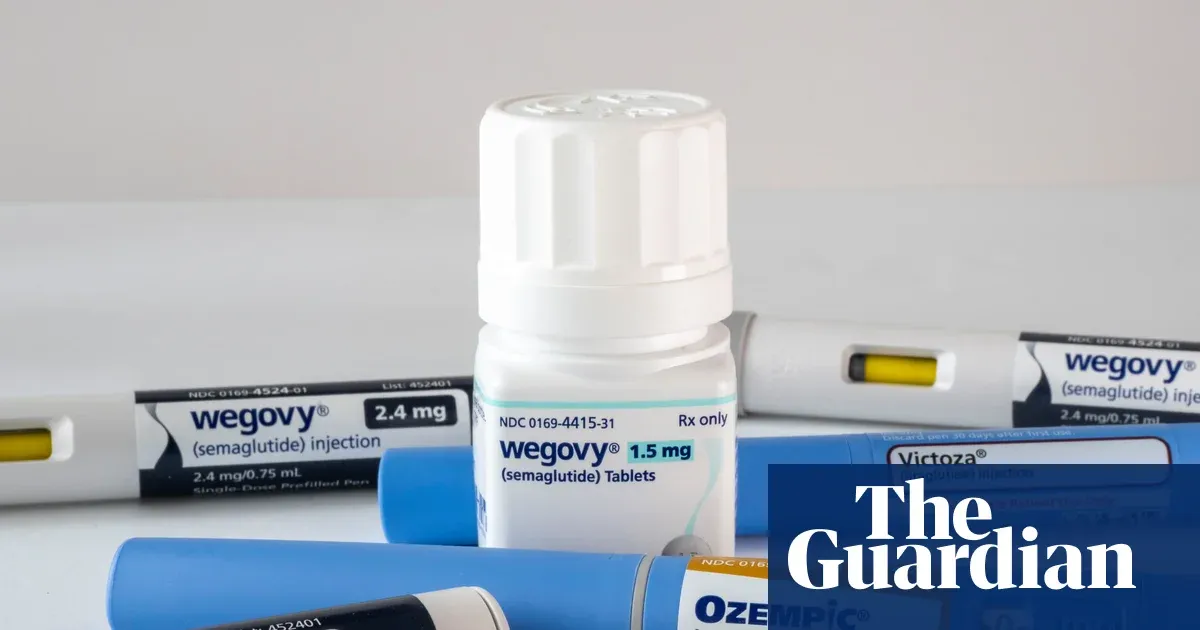
A billion people live with obesity worldwide, and most of them can't afford the drugs that work. That's about to change.
New research suggests semaglutide—sold as Wegovy for weight loss and Ozempic for diabetes—could be manufactured for roughly $3 a month in injectable form, or $16 for a monthly pill. Right now, the same treatment costs $200 in the US and £120 in the UK. The gap isn't about manufacturing complexity. It's about patents and pricing power.
Core patents on semaglutide expire this year in 10 countries including Brazil, China, India, and South Africa. Another 150 countries never had patents filed at all, mostly across Africa. Together, these 160 countries are home to 69% of the world's type 2 diabetes cases and 84% of people living with obesity. Once generics flood the market, the math changes entirely.
We're a new kind of news feed.
Regular news is designed to drain you. We're a non-profit built to restore you. Every story we publish is scored for impact, progress, and hope.
Start Your News Detox"These low prices open the door to worldwide access to an essential medicine," says Dr Andrew Hill, a pharmacologist at Liverpool University who led the analysis. The WHO already designated semaglutide as essential medicine last year—a formal recognition that access shouldn't depend on wealth. The price data, based on 2024-2025 shipment records of key ingredients, uses the same methodology that successfully predicted generic prices for HIV and hepatitis C treatments.
This matters because obesity isn't a rich-world problem anymore. Lower-income countries are shifting to processed foods and sedentary lifestyles faster than their health systems can respond. Diabetes cases jumped from 200 million globally in 1990 to 830 million by 2022, with the steepest rises in low- and middle-income countries. Excess weight contributes to 3.7 million deaths annually.
The Harder Part: Making It Work
But cheaper pills don't solve everything. Dr Nomathemba Chandiwana, a South African obesity specialist, notes that about 27% of adults worldwide meet the criteria for these drugs—and most live in countries with fragile health systems. The real challenge isn't manufacturing cost. It's integration.
These medications work best alongside dietary support, exercise counseling, and treatment for related conditions like heart disease and stroke. They're not a substitute for addressing food insecurity or poverty. They're a tool that only works if health systems have the infrastructure to use it responsibly. That requires coordinated procurement planning, training, and monitoring—the unglamorous work that determines whether a breakthrough actually reaches the people it's meant to help.
The precedent exists. Generic antiretrovirals for HIV, artemisinin combinations for malaria, and direct-acting antivirals for hepatitis C all became affordable in low- and middle-income countries while allowing manufacturers sustainable profit margins. The playbook works. What's different now is scale: semaglutide could eventually benefit hundreds of millions of people, not millions.
Patent expirations begin in March. The question isn't whether cheap versions will exist. It's whether governments and health organizations will use the window to build the systems that turn affordability into actual access.