Northwestern researchers have grown the first human spinal cord tissue sophisticated enough to test what actually happens after injury — and what might fix it.
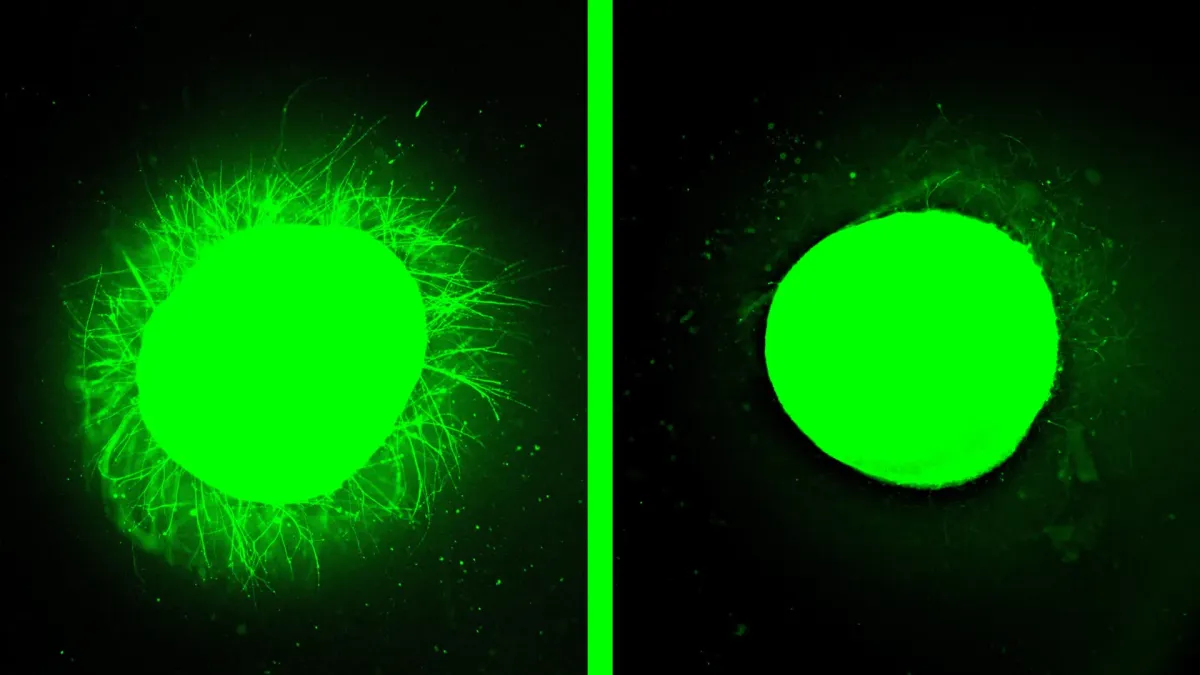
They built these organoids from stem cells, coaxing them over months into miniature spinal cords complete with neurons, support cells, and immune cells. Then they deliberately injured them: some with a scalpel cut, others with crushing pressure, mimicking real spinal cord trauma. Both types produced exactly what happens in actual injuries — cell death, inflammation, thick scar tissue that blocks nerve repair.
Then came the test. The team treated the damaged organoids with "dancing molecules" — a therapy developed by Northwestern's Samuel Stupp that works by moving rapidly through tissue, constantly bumping into cell receptors and triggering the body's natural repair signals. The results were striking. The scar tissue faded to barely visible. Nerve fibers began growing again in organized patterns.
We're a new kind of news feed.
Regular news is designed to drain you. We're a non-profit built to restore you. Every story we publish is scored for impact, progress, and hope.
Start Your News Detox"One of the most exciting aspects of organoids is that we can use them to test new therapies in human tissue," Stupp said. "After applying our therapy, the glial scar faded significantly, and we saw neurites growing, resembling the axon regeneration we saw in animals."
This matters because it's the first time anyone has shown this therapy works in actual human tissue — not just mouse models. The dancing molecules are part of a class of drugs that form a gel scaffold mimicking the spinal cord's natural structure. By adjusting how quickly the molecules move within that scaffold, Stupp's team found faster motion works better. Think of it like this: if the molecules are sluggish, they might never encounter the cells they need to activate. If they're moving, they keep making contact.
In previous animal studies, a single injection 24 hours after severe injury let mice walk again within four weeks. That's the kind of recovery spinal cord injury patients rarely experience — most injuries result in permanent paralysis.
The organoid model itself is a breakthrough. Earlier attempts at growing spinal cord tissue were too simple to show what actually happens after injury. This team was the first to include microglia — the immune cells that drive inflammation in the spinal cord — making the model realistic enough to predict whether treatments will work in humans.
The next phase is harder. Researchers want to build organoids that model chronic injuries, the kind that have been scarred over for months or years. They're also working toward personalized medicine: growing implantable tissue from a patient's own stem cells, which would eliminate the risk of immune rejection.
None of this means paralyzed people will walk again tomorrow. But it does mean researchers can now test spinal cord therapies in human tissue before risking human trials — and the dancing molecules therapy has already shown it can work.