Your chances of catching a cold—and how miserable it feels—may depend more on your body than on the virus itself.
When rhinovirus, the leading cause of the common cold, infects the lining of your nose, something immediate happens. Cells in your nasal passages don't wait for backup. They activate a coordinated defense system designed to stop the virus before it spreads. A new study published in Cell Press Blue shows this cellular response often determines whether you get sick at all, and how bad it gets.
Researchers at Yale School of Medicine grew human nasal tissue in the lab to watch this defense in action. They cultured nasal stem cells for four weeks, exposing the upper surface to air until the cells developed into something that closely resembles the actual lining of your nose and airways. The resulting tissue included mucus-producing cells and cells with cilia—those tiny hair-like structures that sweep mucus out. This matters because rhinovirus only infects humans; traditional lab models using animal cells or simple cell lines miss what actually happens in your body.
We're a new kind of news feed.
Regular news is designed to drain you. We're a non-profit built to restore you. Every story we publish is scored for impact, progress, and hope.
Start Your News Detox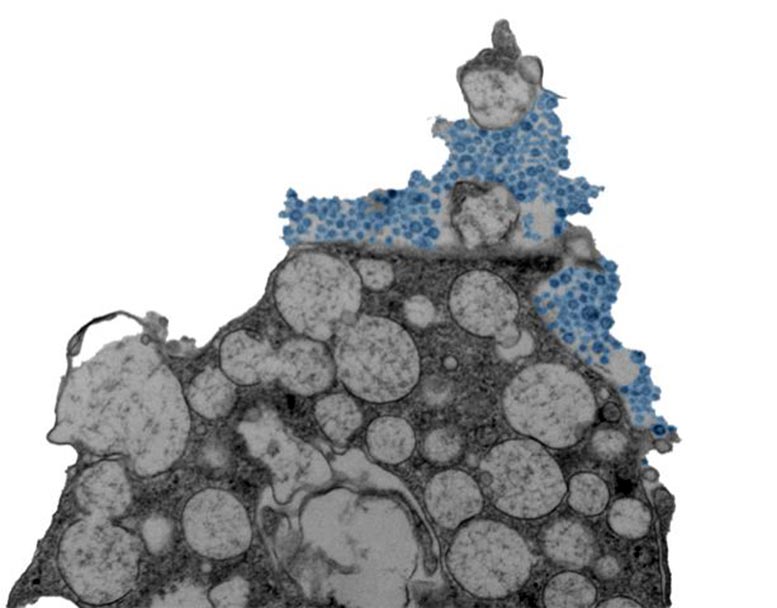
Electron micrograph showing a human nasal epithelial cell releasing rhinovirus (blue). Credit: Julien Amat & Bao Wang
The frontline defense
Watching thousands of cells respond simultaneously, the team discovered a powerful protective system driven by interferons—proteins that prevent viruses from entering cells and replicating. When nasal cells detect rhinovirus, they release interferons that activate antiviral defenses in infected cells and nearby healthy ones. This creates an environment hostile to viral spread. If this response starts quickly enough, the virus gets stopped before it can establish itself.
When researchers experimentally blocked this interferon response, the virus spread rapidly through the tissue, damaging and sometimes killing cells. The takeaway was stark: this early, local defense works—even without any immune cells present. Your nose is doing the heavy lifting before your immune system even gets called in.

Electron micrograph of differentiated human nasal epithelial organoids with cilia of multiciliated cells accentuated in blue. Credit: Julien Amat & Bao Wang
But there's a catch. When viral replication increases despite this first line of defense, your cells activate a secondary response that produces large amounts of mucus and inflammatory signals. This is why you feel congested and miserable—it's your body's attempt to contain the virus, but the inflammation itself causes symptoms. Understanding this distinction opens a new therapeutic angle: treatments that reduce harmful symptoms while keeping the antiviral defenses intact.
The researchers acknowledge their organoid system doesn't capture everything that happens in a real infection. In your actual nasal passages, immune cells arrive to join the fight, and other environmental factors come into play. But this study shifts how we think about colds. The virus isn't the only actor on stage—your body's response to it may be the more important one. That suggests future treatments could focus less on killing the virus and more on optimizing how your cells defend themselves.
For someone with asthma or chronic lung conditions, where rhinoviruses trigger serious breathing problems, this distinction could be significant. It means the path forward might not be about developing antivirals, but about supporting your body's own frontline defenses.